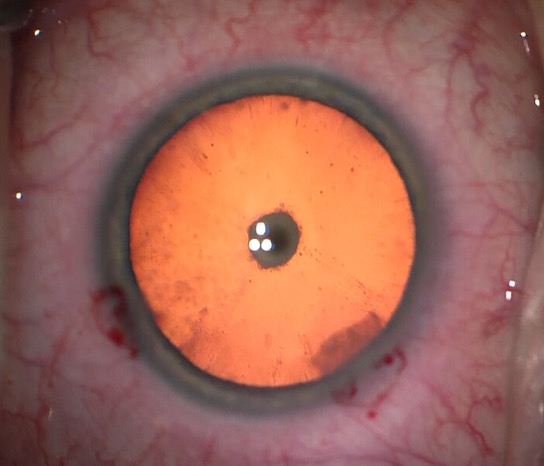
If you are one of the millions of people who suffer from a posterior subcapsular cataract, you may be wondering if surgery is the right option for you. This type of cataract is located in the back part of the lens and can cause several vision problems. In this blog post, we will discuss all aspects of posterior subcapsular cataracts, including signs, causes, impacts, and treatment options. We hope that this information will help you make an informed decision about your treatment options.
What Is Posterior Subcapsular Cataract?
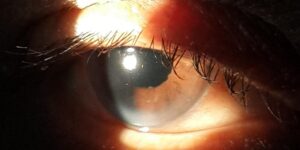
Posterior subcapsular cataracts (PSC) form on the back surface of the lens, nearest your eye’s retina. They are more common in people with diabetes and those who take high doses of steroids for other conditions. PSCs can also run in families.
PSCs usually grow slowly and don’t affect your vision much at first. But as they grow, they can cause many complications
PSCs are different from nuclear cataracts, which form in the center of the lens, or cortical cataracts, which form on the sides of the lens. All three types of cataracts can occur at the same time. You might hear your doctor call a PSC a “subcapsular” cataract. “Subcapsular” means “beneath the capsule.” The capsule is the clear outer covering of your eye’s lens.
This type of cataract is also different from an “after-cataract,” which is a clouding of the eye’s lens that can happen after you have surgery to remove a cataract.
PSC was first described in 1864 by Jaeger, who reported a patient with a posterior subcapsular opacity associated with myopia and cataract surgery. In 1912, de Schweinitz further characterized the clinical features of this entity, noting the association with myopia, cataract surgery, and family history. nuclear sclerosis. The term “posterior subcapsular cataract” was first used in 1966 by Gelineau and colleagues.
From then on, many case reports and small case series of PSC have been published in the literature. In a large population-based study from the United Kingdom, the prevalence of PSC was found to be 0.14% in those younger than 70 years and 0.86% in those older than 70 years. A similar study from Iceland reported a prevalence of 0.16%. Studies from Denmark and Australia have reported prevalences of 0.23% and 0.24%, respectively
PSC is slightly more common in women than several risk factors, including myopia, diabetes mellitus, prolonged use of topical steroids, atopic keratitis, retinitis pigmentosa, uveitis, trauma, previous cataract surgery, and familial predisposition.
PSC typically presents as a unilateral, slowly progressive visual impairment that is often asymptomatic in its early stages. patients usually present with decreased vision and some complaints of glare or halo around lights. As the cataract progresses, symptoms may include decreased night vision, photophobia, and monocular diplopia.
Signs of Posterior Subcapsular Cataract
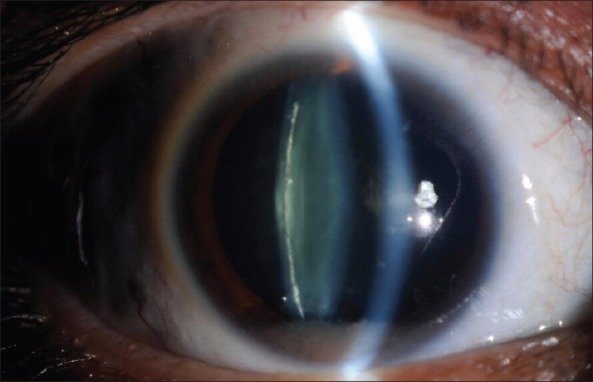
Several signs can indicate you have a posterior subcapsular cataract, which includes:
Glare or halos around
One of the most common signs is glare or halos around light, especially when driving at night. This is because the back of the lens becomes clouded, which affects your ability to focus on light. Sometimes there may be many tiny dots of light in your vision.
Blurry Vision
Another sign is blurred vision. If the cataract has not yet formed, you may experience double vision in that eye. If it has fully formed, then your central vision will be blurry while your peripheral (side) vision remains clear.
Frequent Changes In Eyeglass Prescription
If you notice that you have to change your eyeglass or contact lens prescription more frequently than usual, it could be a sign of a posterior subcapsular cataract. This is because the clouding of the back of the lens affects how light enters your eye, which then changes how you see.
Sensitivity To Light
If you have a posterior subcapsular cataract, you may also be more sensitive to light than usual. This means that you may steel disc bright lighting conditions. This sensitivity can also make it difficult to read.
Constant Need For Light
If you find that you need more and more light to read, it may be a sign that you have a posterior subcapsular cataract. This is because the clouding of the back of your lens makes it difficult for light to reach your retina, which is the part of your eye that processes images.
Needing To Change Your Reading Position
If you have a posterior subcapsular cataract, you may find that you need to hold your book or newspaper closer to your face than usual to see it. This is because the cloudiMany risk factors can difficult for light to reach your retina.
Shadow Over Your Vision
As the cataract grows, it may cast a shadow over your central vision. This can make it difficult to see clearly, especially when looking at objects that are light in color. Sometimes these also appear as dark spots in your vision.
If you notice any of these signs, it is important to see an eye doctor for a comprehensive eye exam. They will be able to determine if you have a posterior subcapsular cataract and recommend the best treatment options for you.
Risk Factors For Posterior Subcapsular Cataract

Many risk factors can contribute to the formation of a posterior subcapsular cataract. Some of these include:
Advanced age
One of the most significant risk factors for the development of a posterior subcapsular cataract is advanced age. As we age, the proteins in our lenses begin to break down and clump together, which can cause the formation of a cataract. Sometimes there may be many tiny dots of light in your vision.
Diabetes
People with diabetes are also at an increased risk of developing a posterior subcapsular cataract. This is because high levels of sugar in the blood can damage proteins in the lens, which can lead to the formation of a cataract. Sometimes diabetes also causes changes in the shape of the lens, which can also lead to a posterior subcapsular cataract.
Prolonged exposure to ultraviolet (UV) light
Exposure to UV light is another risk factor for the development of a posterior subcapsular cataract. This is because UV light can damage proteins in the lens, which can lead to the formation of a cataract. Prolonged exposure to sunlight or other sources of UV light (such as tanning beds) can increase your risk of developing a posterior subcapsular cataract.
Previous eye surgery
People who have had previous eye surgery are also at an increased risk of developing a posterior subcapsular cataract. This is because the incision made during surgery can damage the lens and lead to the formation of a cataract.
Corticosteroid Use
People who take corticosteroids are also at an increased risk of developing a posterior subcapsular cataract. This is because corticosteroids can damage proteins in the lens, which can lead to the formation of a cataract. Corticosteroid use includes both oral and topical forms (such as eye drops).
Certain Medications
Another risk factor for the development of a posterior subcapsular cataract is the use of certain medications. These include:
- Tricyclic antidepressants
- Calcium channel blockers
- Sulfonamide antibiotics
- Chloroquine (an anti-malarial medication)
If you are taking any of these medications, it is important to speak with your doctor about the risks and benefits of continuing treatment.
Gender
Another risk factor that can be associated with the development of a posterior subcapsular cataract is gender. Studies have shown that women are more likely to develop this type of cataract than men.
Race
There is also a difference in the incidence of posterior subcapsular cataracts among different races. Studies have shown that Caucasians are more likely to develop this type of cataract than people of other races.
While there are many risk factors for the development of a posterior subcapsular cataract, it is important to remember that not everyone who has one or more of these risk factors will develop a cataract.
How Does Posterior Subcapsular Cataract Impacts Someone?
Positively, a posterior subcapsular cataract does not impact one’s vision as much as nuclear sclerosis or cortical cataracts. This is due to the location of the cataract, which is towards the back of the eye. Posterior subcapsular cataracts tend to grow slowly and have few symptoms in the early stages.
Negatively, when left untreated, posterior subcapsular cataracts can cause vision loss and make it difficult for someone to see clearly. In addition, this type of cataract can be more difficult to treat than other types of cataracts because it is located in a hard-to-reach area of the eye. As a result, surgery may be needed to remove the cataract and restore vision.
Sometimes these negative impacts can be mitigated by taking certain precautions, such as wearing sunglasses or using eye drops. However, in most cases, surgery will eventually be necessary to correct the problem. If you think you may have a posterior subcapsular cataract, it is important to see an ophthalmologist so that they can diagnose and treat the condition.
Diagnosis of Posterior Subcapsular Cataract
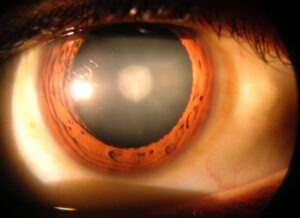
Diagnosis of posterior subcapsular cataracts can be difficult. Often, there are no obvious symptoms until the cataract has progressed and vision is affected. A comprehensive eye examination by your ophthalmologist is the best way to determine if you have a cataract.
Your ophthalmologist will look for changes in the lens of your eye during an eye exam. He or she may use a special magnifying lens, shine a light into your eye, or both. If you have a cataract, you may see one or more of the following:
- Cloudiness or haziness in your vision
- Difficulty seeing at night
- glare from lights
- Double vision in one eye
- Fading or yellowing of colors
- Frequent changes in your eyeglass prescription
If you have any of these symptoms, contact your ophthalmologist. He or she will perform a comprehensive eye examination to determine if you have a cataract and, if so, what type it is. There are some tests like the A-Scan that can help determine the size and shape of your cataract.
Posterior subcapsular cataracts tend to grow slowly and may not cause symptoms for years. For this reason, regular comprehensive eye examinations are important, especially if you are age 60 or have diabetes. If you have a family history of cataracts, should also have regular eye exams. Early diagnosis and treatment of cataracts are important to vision.
Treatment of Posterior Subcapsular Cataract

Treating posterior subcapsular cataracts usually involves surgery to remove the cloudy lens and replace it with an artificial lens. This type of surgery is called cataract surgery.
Cataract Surgery
Cataract surgery is one of the most common types of surgery performed today. More than three million people have cataract surgery each year. Cataract surgery is usually successful in improving vision. In most cases, it corrects vision enough so that people don’t need to wear eyeglasses or contact lenses after surgery.
The surgeon makes a tiny incision in your eye and inserts a small instrument called a phacoemulsification probe. The probe emits ultrasound waves that break up the cloudy lens so it can be suctioned out. The surgeon then inserts an intraocular lens (IOL) into the space where the natural lens was removed.
Most cataract surgeries are performed on an outpatient basis, which means you don’t have to stay in the hospital overnight. The surgery usually takes less than 30 minutes. You will need someone to drive you home after the surgery.
Recovery from cataract surgery is usually quick. Most people notice a significant improvement in their vision within a few days or weeks after surgery. In some cases, however, it may take longer for your vision to improve.
Other treatment options that can be used to treat posterior subcapsular cataracts include:
- Focal therapy: This treatment involves using a laser to destroy the cloudy areas of the lens. It is not yet approved by the FDA for treating cataracts, but it is being studied in clinical trials.
- Vitrectomy: This surgery involves removing the vitreous, or jelly-like substance, from the center of your eye. This can be done if the cataract is located behind the vitreous. It also may be used if cataract surgery cannot be performed because of other medical problems. If you have a posterior subcapsular cataract, talk to your ophthalmologist about the best treatment option for you.
- Eye Drops: An eye drop called N-acetyl carnosine (Can-C) has been shown to slow the progression of cataracts. It is available without a prescription in some countries, but it is not yet available in some countries
Conclusion
Cataract surgery is a relatively safe and effective way to improve vision. Posterior subcapsular cataracts are a common type of cataract and can be treated effectively with surgery. If you have a posterior subcapsular cataract, talk to your doctor about whether surgery is right for you.
People who have a cataract in the back of their eye (a posterior subcapsular cataract) may notice that their vision becomes worse when they look at bright lights. This type of cataract is common, and it can be treated effectively with surgery.
If you have a posterior subcapsular cataract, talk to your doctor about whether surgery is right for you. Surgery is generally safe and effective, and it can help improve your vision.
Cataract surgery is a safe and painless procedure. At EyeMantra we have a team of experienced eye surgeons, who will be happy to answer your any questions on cataract surgery, cataract surgery cost, cataract lens cost for different cataract surgery types- Phacoemulsification, MICS & Femto Laser Cataract. Call us at +91-9711116605 or email at [email protected] for inquiries.